-
 By John S. King, MD
By John S. King, MD
Retina Associates, PA - Uploaded on Nov 17, 2019.
- Last modified by John S. King, MD on Nov 22, 2019.
- Rating
- Appears in
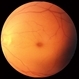
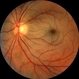
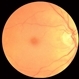
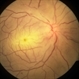
- Moyamoya CRAO with CRA Sparing OD and NVI
- Condition/keywords
- moyamoya, central retinal artery occlusion (CRAO), cilioretinal sparing, neovascularization of iris (NVI)
- Photographer
- Gretchen Harper
- Imaging device
-
Fundus camera
Topcon - Description
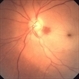
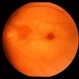
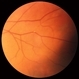
- 60-year-old white female presented with five days of acute vision loss in the right eye. She was seen initially by referring doctor after hours five days ago and diagnosed with a CRAO and sent to ED to be evaluated stroke team. Right ICA was 100% closed but completely bypassed. She called four days later c/o redness and eye pain; at this point prominent iris vessels were seen, and she was sent to us. Her background history includes a diagnosis of moyamoya (underwent bilateral cerebral artery bypass 2015); atorvastatin for hypercholesterolemia; ASA; no hx of HTN or heart disease. She had a scleral buckle repair OD in 2017 and later developed a thick ERM, which was repaired in 2018; on her previous visit her acuity was noted at 20/40. On presentation her visual acuity was HM OD and 20/15 OS. IOP was 8 OD and 10 OS. There were prominent iris vessels in the right eye, no cell or flare, and an IOL. The posterior segment exam showed diffuse retinal whitening with attenuated vessels and boxcarring; there was sparing retinal whitening in a central area of the macula that appeared to be supplied by a cilio-retina artery. The FA showed very slow filling of the retinal vessels; there was some early perfusion secondary to the cilio-retinal artery. At 7 minutes there was still significant areas of non-perfusion, as well as macular ischemia. Avastin was administered, and one week later, PRP was performed. On the day PRP was performed, the irregular iris vessels had regressed completely. She said that she had a "sliver" of vision centrally in that eye; her acuity was CF 2' and IOP 12.


 Initializing download.
Initializing download.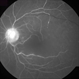

---thumb.jpg/image-square;max$79,0.ImageHandler)